Diverticulitis: Symptoms, Diet & Treatment Guide
Stomach pain is a universal experience. In India, we often dismiss abdominal discomfort as the aftermath of a heavy, spicy meal. We blame the extra helping of biryani or a late-night street food snack. We take an antacid, drink some warm ajwain water, and hope the problem simply fades away. Sometimes it does. Often, however, a persistent, localized pain signals a structural change happening deep inside the large intestine.
The human digestive tract is a resilient system, capable of processing decades of diverse dietary inputs. Yet, it has its breaking points. When the muscular walls of the colon face years of immense pressure—often due to low-fiber diets and chronic constipation—they begin to yield. Tiny, balloon-like pouches form. This structural alteration is the beginning of a complex physiological cascade that can impact your entire body, extending far beyond simple indigestion.
Understanding how these intestinal changes occur, how they provoke your immune system, and exactly what to put on your plate to heal is essential. We will explore the science of gut inflammation, the specific phases of recovery, and the medical interventions available today.
The Anatomy of the Problem: What Exactly is Happening in Your Gut?
To comprehend the severity of abdominal pain, you must first understand the architecture of your colon. The large intestine is a muscular tube responsible for absorbing water and pushing waste out of the body. To do this effectively, it relies on coordinated muscle contractions known as peristalsis.
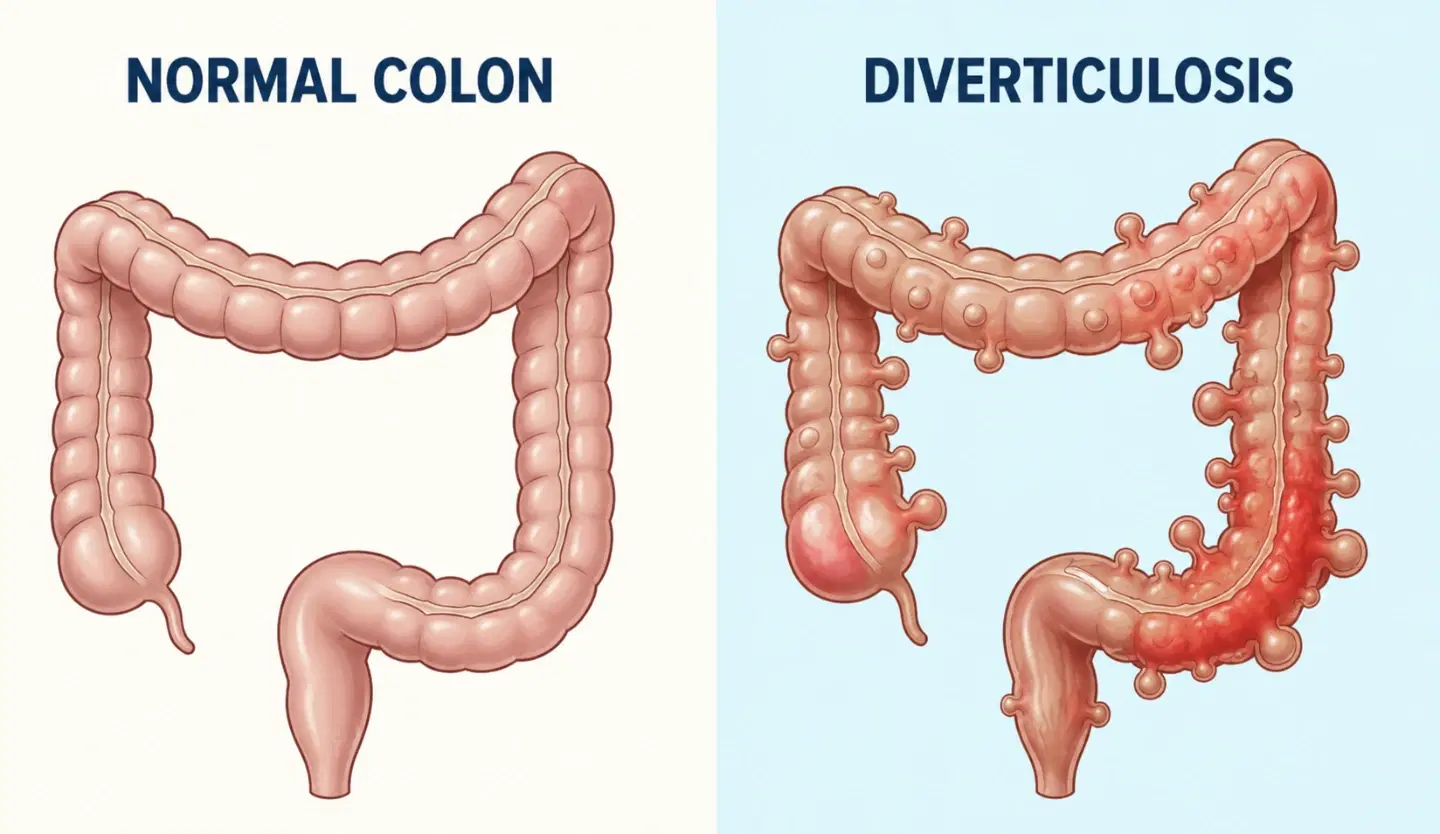
When your diet lacks sufficient dietary fiber, your stool becomes hard and difficult to pass. The colon has to strain aggressively. Over time, this intense internal pressure pushes against the weakest points in the intestinal wall. The inner lining bulges through the muscle layer, creating small, marble-sized pouches.
The presence of these pouches is referred to clinically as diverticular disease. Having the pouches without any active inflammation or infection is called diverticulosis. Most people with diverticulosis walk around entirely unaware of their condition. They experience zero symptoms. It remains a silent structural anomaly.
The crisis begins when these pouches become inflamed or infected. If you find yourself asking, "What is diverticulitis?" the answer lies in this precise transition. When microscopic tears occur in the walls of these pouches, or when fecal matter and harmful bacteria become trapped inside them, a severe localized infection erupts. This inflamed, infected state is diverticulitis.
Think of the colon wall like a busy Indian highway. Years of heavy wear and tear cause the asphalt to weaken, forming deep potholes (diverticulosis). As long as traffic flows around them, the road functions. However, if debris gets jammed into a pothole and damages the underlying structure, causing a massive traffic blockade and requiring emergency repair crews, you have an active crisis (diverticulitis).
Recognizing the Warning Signs: Symptoms You Cannot Ignore
The transition from a silent pouch to an active infection is rarely subtle. The body sounds an alarm. Recognizing these signals early can prevent severe complications, such as abscesses, intestinal blockages, or a ruptured colon.
The most prominent symptom is sharp, constant pain. In Western populations, this pain almost always localizes in the lower left side of the abdomen. However, due to anatomical and genetic variations, it is well-documented that patients in Asian countries, including India, frequently experience this pain on the right side. This right-sided pain can easily be mistaken for appendicitis, making professional medical imaging vital.
Alongside severe pain, you may experience:
- A sudden, unexplained fever accompanied by chills.
- Profound nausea and occasional vomiting.
- Drastic changes in bowel habits, usually presenting as severe constipation, though diarrhea can also occur.
- Bloating and extreme tenderness when the abdomen is touched.
Ignoring these symptoms is dangerous. A minor infection can rapidly escalate into a life-threatening abdominal emergency. If you are experiencing chronic or severe abdominal issues, educating yourself on potential underlying conditions is the first step toward healing. For a detailed breakdown of warning signs, read about Repeated Stomach Pain: Hidden Causes You Shouldn’t Ignore.
The Gut-Immune Connection: Inflammation, the Microbiome, and Joint Health
To truly understand digestive diseases, we must look beyond the colon. The human gut is not merely a digestive pipe; it is the headquarters of your immune system. Nearly 70% of your immune cells reside in the gut-associated lymphoid tissue (GALT). This means that local inflammation in the intestines rarely stays local.
The Microbiome's Role in Systemic Health
Your large intestine is home to trillions of bacteria, fungi, and viruses, collectively known as the gut microbiome. In a healthy state, these microbes live in symbiosis with you. They ferment dietary fiber to produce short-chain fatty acids (SCFAs), like butyrate, which keep the intestinal lining strong and regulate the immune system.
When diverticular disease progresses into an active infection, this delicate microbial balance is shattered. Pathogenic bacteria multiply rapidly inside the inflamed pouches. This state of imbalance is called gut dysbiosis. The structural integrity of the intestinal wall degrades. The tight junctions holding the intestinal cells together begin to loosen, resulting in increased intestinal permeability, commonly referred to as "leaky gut."
How Gut Inflammation Triggers the Autoimmune Response
Once the intestinal barrier is compromised, toxins, undigested food particles, and bacterial lipopolysaccharides (LPS) leak directly into the bloodstream. Your immune system spots these foreign invaders and launches a massive, systemic attack.
This is where the connection between gut health and autoimmune diseases becomes apparent. A healthy immune system targets specific threats and then stands down. A confused immune system, constantly bombarded by toxins leaking from a compromised gut, stays locked in a hyperactive state.
Imagine chaotic Indian city traffic at a major intersection when the traffic lights suddenly stop working. Vehicles rush from all sides, horns blaring, causing massive gridlock and accidents. Your immune system acts similarly during chronic inflammation or an autoimmune flare-up. It loses its signaling mechanisms. In the confusion, instead of just attacking the leaked bacteria, it begins attacking your body’s own healthy tissues.
The Gut-Joint Axis
This systemic confusion explains why chronic gut inflammation frequently manifests as severe joint pain. The proteins found in the walls of certain gut bacteria look structurally similar to the proteins found in human joint tissue. Through a process called molecular mimicry, the antibodies your body creates to fight the gut infection end up attacking your knees, wrists, and spine. This mechanism links severe gut disorders directly to autoimmune conditions like rheumatoid arthritis and ankylosing spondylitis [Source: Journal of Autoimmunity].
Healing the physical structure of the colon and restoring the microbiome is therefore not just about stopping stomach pain. It is about calming the entire central immune response and protecting the rest of your body from systemic inflammatory damage.
Structuring the Perfect Diverticulitis Diet: A Phased Approach
Food is your primary tool for modulating gut inflammation. However, the right food at the wrong time can worsen the condition. A proper diverticulitis diet is not a static list of rules; it is a phased approach that changes based on the active state of your colon.
Managing what you eat requires patience. You must transition your digestive system slowly from a state of complete rest to a state of high-fiber resilience.
Phase 1: Complete Bowel Rest (The Clear Liquid Diet)
When an infection is actively raging, your colon needs to stop working. Digestion requires intense muscular contractions. You need to temporarily halt these contractions. For the first two to three days of an acute attack, a doctor will likely prescribe a strict clear liquid diverticulitis diet.
The goal here is simple hydration and basic caloric intake without leaving any residue in the colon.
- What to consume: Water, clear coconut water (nariyal pani), light vegetable broths, and very thin, strained dal water (the clear liquid on top of cooked lentils, completely devoid of solid matter).
- What to avoid: Milk, juices with pulp, thick soups, and absolutely all solid food.
Phase 2: Gentle Reintroduction (The Low-Residue Diet)
Once the sharp pain subsides and your fever drops, you can slowly reintroduce solid foods. However, this is not the time for heavy fiber. You need low-residue foods that digest quickly and pass through the colon without leaving bulky waste that could get trapped in the healing pouches.
During this middle phase, your diverticulitis diet should consist of easily digestible, soft foods commonly found in an Indian kitchen.
- Ideal foods: White rice (highly polished, not brown rice), very soft plain khichdi made with moong dal and white rice, idli, boiled potatoes without the skin, and well-cooked, pureed carrots.
- Protein: Lean, easily digested proteins like plain yogurt (curd), eggs, or boiled chicken.
- Spices: Keep it minimal. A pinch of turmeric and salt is fine. Avoid red chili powder, garam masala, and raw garlic, which can irritate the healing mucosal lining.
Phase 3: The Long-Term Maintenance Strategy (The High-Fiber Diet)
Once you are completely pain-free and cleared by your gastroenterologist, the strategy shifts entirely. To prevent future attacks of diverticular disease, you must build a robust, bulky stool that keeps the colon expanded and prevents pressure build-up. This requires a high-fiber diverticulitis diet.
You must add fiber gradually. Adding 30 grams of fiber overnight to a digestive system that has been resting will cause severe bloating and gas. Add a few grams every few days, and aggressively increase your water intake. Fiber without water acts like concrete in the gut; fiber with water acts like a soft sponge.
Building a high-fiber Indian diet:
- Grains: Transition from white rice to whole wheat roti, oats, brown rice, and millets like ragi or jowar.
- Legumes: Lentils (dals), chickpeas (chana), and kidney beans (rajma) are phenomenal sources of both soluble and insoluble fiber.
- Vegetables: Load up on leafy greens, spinach (palak), bottle gourd (lauki), and ridge gourd.
Patients frequently ask specific dietary questions. For instance, "Can you eat okra with diverticulitis?" The answer is yes, absolutely, once you are fully recovered. Okra (bhindi) is rich in mucilaginous soluble fiber, which is exceptionally soothing to the digestive tract and helps feed beneficial gut bacteria. However, you should avoid it during the acute Phase 1 or Phase 2.
Clarifying Outdated Dietary Advice
Historically, doctors handed out strict lists of foods to avoid with diverticulitis, firmly banning nuts, seeds, popcorn, and tomatoes. The theory was that tiny seeds would physically get stuck inside the pouches and trigger an infection.
Modern gastroenterology has comprehensively debunked this myth [Source: American Gastroenterological Association]. Current research shows no link between eating nuts or seeds and an increased risk of developing an infection. In fact, because nuts and seeds are high in fiber, avoiding them might actually increase your risk of an attack. You can enjoy your almonds, chia seeds, and tomatoes without fear, provided you chew them thoroughly and are not currently experiencing an active flare-up.
For more insights on optimizing your gut function and choosing the right ingredients for your daily meals, Eat These Fantastic Foods for a Healthy Small Intestine!
Advanced Diagnostics and Medical Treatment
While a highly structured diverticulitis diet is the foundation of management, medical intervention is often necessary. You cannot treat a severe internal abdominal infection solely with diet.
Diagnostic Procedures
When you present with severe abdominal pain, a physician cannot guess the cause. They must look inside. Blood tests are immediately drawn to check your white blood cell count and C-Reactive Protein (CRP) levels, which indicate the severity of the systemic infection.
The gold standard for diagnosing an acute flare-up is a Computed Tomography (CT) scan of the abdomen and pelvis. A CT scan gives doctors a precise 3D map of your colon. It shows exactly where the inflamed pouches are, whether there are any dangerous abscesses forming, and if the bowel wall has thickened.
A colonoscopy is generally avoided during an acute attack. Inserting a scope into a highly inflamed, weakened colon carries a significant risk of causing a perforation. However, six to eight weeks after the infection has fully resolved, a follow-up colonoscopy is mandatory to rule out colon cancer and assess the extent of the diverticular disease.
At specialized centers like Bangalore Gastro Centre, advanced diagnostics help identify the exact location and severity of the inflammation, ensuring a targeted treatment plan rather than relying on guesswork.
Medical and Surgical Interventions
Treatment depends entirely on the severity of the scan results.
- Uncomplicated Cases: Mild infections are often treated at home. A doctor will prescribe a targeted course of oral antibiotics alongside a strict clear liquid diet. Rest is mandated.
- Complicated Cases: If you are unable to keep fluids down, have a high fever, or the CT scan shows an abscess, hospitalization is required. You will receive intravenous (IV) antibiotics and fluids.
- Surgical Options: In cases where an abscess cannot be drained, a perforation occurs, or a patient suffers from multiple, unrelenting attacks every year, surgery becomes necessary. A surgeon will perform a bowel resection (colectomy), physically removing the diseased segment of the colon and reattaching the healthy ends. Modern surgical techniques often allow this to be done laparoscopically, significantly reducing recovery time.
Patient Questions: Deep Dive into Autoimmunity and Gut Health
When dealing with chronic digestive issues, patients often have concerns that extend beyond basic dietary advice. Understanding the systemic impact of gut health is essential for long-term well-being.
What triggers autoimmune diseases?
Autoimmune diseases occur when the immune system loses its ability to distinguish between foreign pathogens and the body's own healthy tissue. While genetics play a base role in susceptibility, environmental factors are the primary triggers. The most significant environmental trigger is a compromised gut microbiome. Viral infections, chronic high-stress levels, exposure to specific environmental toxins, and a poor diet heavily heavily laden with ultra-processed foods all contribute. When these factors combine, they can flip the genetic switch, initiating the autoimmune response.
How does gut inflammation trigger an autoimmune flare-up?
The mucosal lining of your gut is a tightly regulated security gate. When chronic inflammation (from conditions like severe diverticular disease or general dysbiosis) damages this lining, the tight junctions between cells break open. This "leaky gut" allows lipopolysaccharides (LPS), harmful bacteria, and undigested proteins to flood into the bloodstream. The immune system detects these foreign bodies in the blood and mounts a massive inflammatory response. Because this immune response is systemic rather than localized, it frequently attacks vulnerable tissues elsewhere in the body, triggering a widespread autoimmune flare-up.
How does the gut microbiome specifically play a role in joint health?
The connection lies in a concept called molecular mimicry and the migration of inflammatory cells. When pathogenic bacteria overgrow in the gut, the immune system generates specific antibodies to destroy them. Unfortunately, the protein sequences on the surface of some of these gut bacteria closely resemble the proteins found in the synovial fluid of human joints. The antibodies mistake your joint tissue for the gut bacteria and attack it. Furthermore, inflammatory cytokines produced in the inflamed gut can travel through the bloodstream directly to the joints, causing swelling, stiffness, and severe pain characteristic of reactive arthritis.
Is an optimal diverticulitis diet the same for everyone?
No. The phases of the diet (liquid, soft, high-fiber) are universally applicable, but the specific foods within the maintenance phase must be personalized. Every individual's microbiome is unique. While one person may digest raw spinach perfectly, another might experience severe bloating. A successful high-fiber diverticulitis diet requires careful experimentation. You must introduce new fibrous foods slowly, track your bodily responses, and consult with a clinical dietitian to ensure you are getting adequate nutrition without triggering spasms.
When should I see a gastroenterologist for stomach pain?
Do not wait for pain to become unbearable. You should seek immediate consultation with a specialist if you experience sharp, localized pain that does not subside within a few hours, especially if it is accompanied by a fever above 100.4°F (38°C). Furthermore, if you notice unexplained weight loss, blood in your stool (which can appear bright red or very dark and tarry), or a sudden, drastic shift in your normal bowel habits lasting more than a few days, medical evaluation is required. Early intervention prevents mild inflammation from turning into an emergency requiring surgical bowel resection.
Conclusion
Managing the health of your colon is a lifelong commitment. The transition from a silent structural weakness to a painful, active infection is heavily influenced by your daily choices. While genetics and age play their part in weakening the intestinal walls, your lifestyle holds the key to prevention.
By understanding the physiological mechanics of your gut, recognizing the early warning signs of inflammation, and respecting the powerful connection between your microbiome and your systemic immune system, you take control of your health. Implement a thoughtful, progressive diverticulitis diet, prioritize hydration, and never ignore persistent abdominal pain. With the right dietary adjustments and expert medical guidance from facilities like Bangalore Gastro Centre, you can heal your gut, quiet systemic inflammation, and return to a vibrant, pain-free life.
